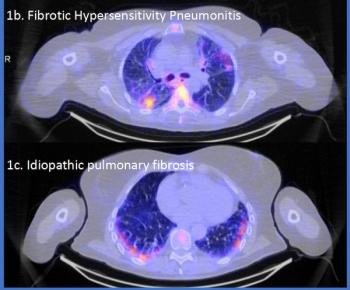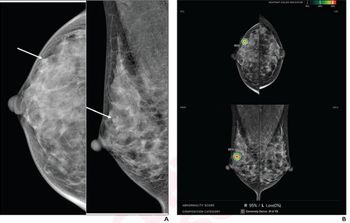
Non-Ferromagnetic Bullets Leave Traces, Indicating They Are Safe for MRI
Radiologists can use X-rays and CT scans to identify features left by non-ferromagnetic ballistic fragments, opening the door to MRI imaging for some patients.
With the help of either X-ray or CT scans, radiologists can determine whether a patient with embedded bullet fragments can safely undergo an MRI exam, a new study has found.
Typically, patients who have either new or old gunshot wounds are denied imaging with MRI due to both safety and image quality concerns. But, investigators from Emory University have pinpointed various features visible on X-ray or CT that providers can use to identify whether the fragments are non-ferromagnetic and, therefore, MRI-safe. They published their findings in the
“MRI of patients with retained ballistic objects is frequently avoided because evidence of safety and knowledge regarding ballistic materials are lacking,” said first author Arthur J. Fountain, M.D., associate professor of radiology and imaging sciences at Emory and chief of radiology at Grady Memorial Hospital in Atlanta, noting that quick identification of bullet composition prior to imaging is not always possible. “Dual-energy CT [has been used] to identify the metallic composition of bullets, [but] the modality is not universally available, and expertise is required for image interpretation.”
To date, he said, no other studies examining the appearance of the ballistic bullet trail and the correlation with the behavior of projectiles in the MIR magnetic field have been published. Consequently, Fountain’s team tested the most commonly fired bullets from the most commonly used guns that are associated with wounds that appear most frequently in the clinical environment.
“Our study advances the literature in that bullet penetration was measured and debris trails and ballistic projectile tracks were systematically assessed with radiography and CT, in contrast with earlier studies,” he said.
To evaluate the bullets and search for patterns, his team conducted ballistic testing with solid lead, lead core with full copper-alloy jacket, and alloy-jacket hollow points with or without a polymer plug in the tip bullets, shooting them with semi-automatic pistols and revolvers. Bullets were fired into ballistic gel blocks designed to mimic human tissue.
After firing the bullets, the team captured conventional X-rays of each block on both anteroposterior and lateral projections, as well as CT images acquired with a 64-MDCT scanner at 0.625-mm slices. They also performed T1- and T2-weighted MRI sequences with a 1.5-T scanner on unfired bullets suspended in gelatin blocks, assessing magnetic attractive force, rotational torque, and heating effects of unfired bullets.
Based on their observations and comparisons, the radiologists were able to correctly distinguish ferromagnetic bullets from non-ferromagnetic. The bullets that left a debris track or those that appeared deformed on X-ray and CT were non-ferromagnetic. These fragments were made of copper, copper-alloy, lead composition with a partial jacketed configuration, or shotgun shot.
Such bullets also do not heat up or produce and detectable force or torque during and MRI scan, and artifact was negligible on the T1- and T2-weighted MR images, Fountain said. Specifically, the .45 automatic Colt pistol (ACP) jacket hollow point (JHP), 9-mm Parabellum JHP, .357 Magnum JHP, .38 Special hollow point (HP), and lead shot were non-ferromagnetic.
To test for any temperature changes, the team monitored bullet temperatures for 22 minutes during MRI scans of the bullets and the phantoms. During that time, they did not see any heating above the 2o-degree limit set by the U.S. Food & Drug Administration.
“Non-ferromagnetic ballistic projectiles do not undergo movement or heating during MRI,” the team concluded, “and the imaging modality can be performed when medically necessary without undue risk and with limited artifact susceptibility on the resulting images, even when the projectile is in or near a vital structure.”
Based on these results, Fountain said, his team created an algorithm that radiologists can use to correctly triage imaging for patients who have embedded ballistic fragments. If a review of an X-ray or CT image reveals a debris track or bullet deformation, they can safely release the patient for MRI imaging regardless of when the injury occurred.
In addition, MRI may also be attempted if the projectile matches the characteristics of a BB even when no debris track or deformation is present, but radiologists should anticipate artifact could potentially decrease diagnostic utility. MRI should not be attempted if the radiologist cannot identify a debris track or deformation, Fountain said.
Newsletter
Stay at the forefront of radiology with the Diagnostic Imaging newsletter, delivering the latest news, clinical insights, and imaging advancements for today’s radiologists.